Why AI Will Break Biotech’s Death Spiral
Moore’s Law will crush Eroom’s Law to unblock stagnated biotech.
Foreword:
Earlier this year, Michael Spencer from the AI Supremacy Substack approached me to write a guest article on how AI will impact the field of medicine. After some discussion, we decided to narrow the focus specifically to drug development. The original article was posted a little over a week ago, but I wanted to reshare it with any of my readers who may have missed it. Plus, I felt there were a few updates I could add for fun—it's a fast-moving field!
So, what's the article about?
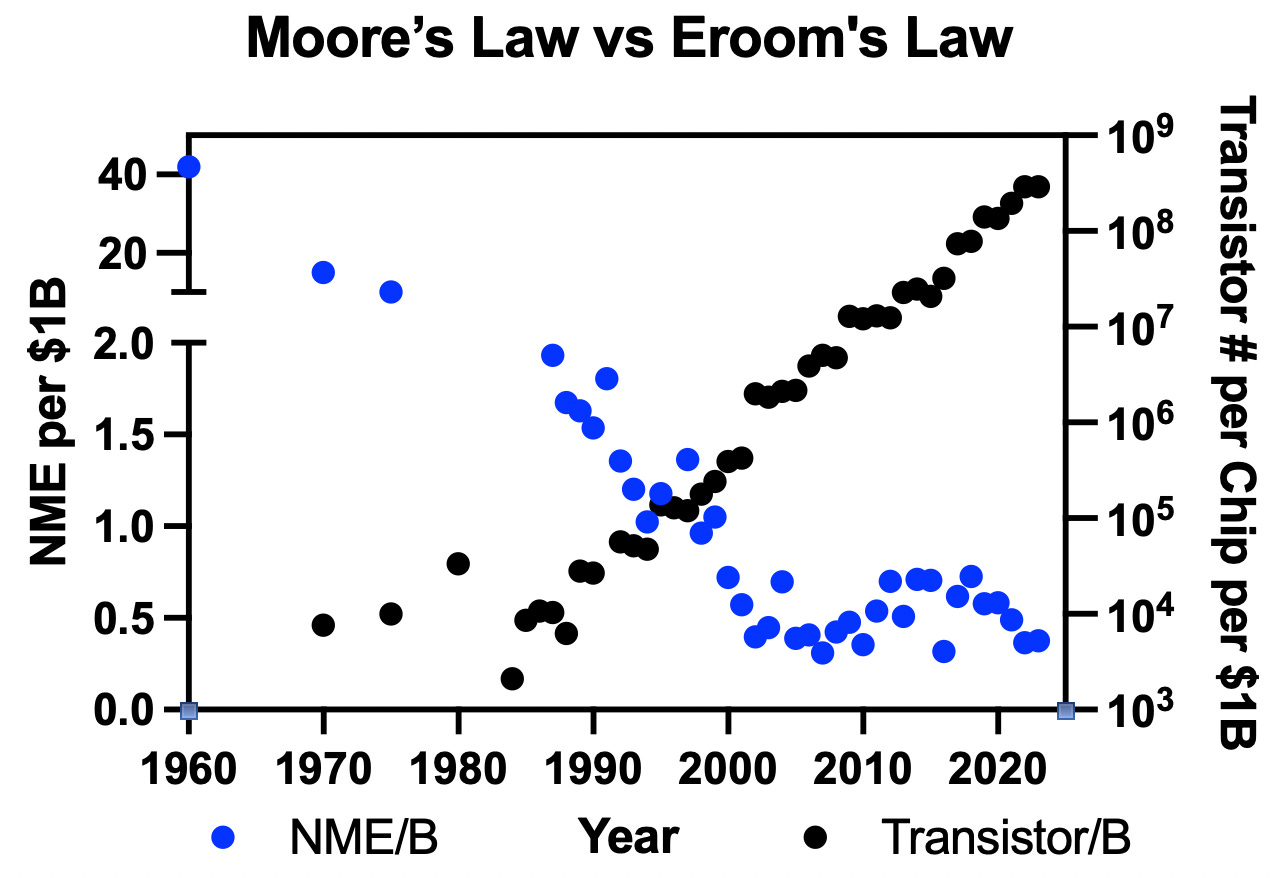
Progress in drug development, measured by new drugs each year, has been slowing decade by decade, with skyrocketing costs. This slowdown and stagnation, which we describe in the article, is often referred to as Eroom's Law. Conversely, the technology field has seen an absolute boom over the past decades, due largely to the number of transistors that can be put onto a microprocessor consistently increasing year by year—a phenomenon known as Moore's Law. This exponential growth has fueled significant advancements in various technological fields, including artificial intelligence and machine learning.
Will leveraging these advancements in traditional technology powered by Moore's Law allow us to reverse the harm of Eroom's Law? This is a metaphorical war between progress and stagnation. In many respects, who wins—Eroom or Moore—will shape the future of humanity. Will the future of medicine become so overly expensive and cumbersome that drug development entirely stalls out? Or will technological developments like generative AI counteract this and enable future prosperity?
Introduction: Why I think Pharma is in crisis and how AI can save it.
Let’s be honest, the biotechnology sector is currently struggling. This is particularly true for Pharmaceuticals. And no, I’m not referring to the COVID-19 vaccine hangover - which certainly isn’t helping anything - but a broader decades-long trend. It’s bitter to say it, especially when I’ve spent my entire life training to be in this field. But there’s no way of getting around this truth. Things won’t get better until we admit there is a problem. What is that issue? There is something fundamentally broken with the traditional drug development pipeline.
Why do I think this?
Well, we are in a time of unprecedented technological development, where our tools are rapidly evolving, enabling high-throughput testing, development, and analytics we never even imagined. With such significant advancements, we would expect to see a matched growth in pharmaceutical development, e.g., many new impactful drugs reaching patients, prices for therapeutics and diagnostics falling, life expectancy increasing, and so on. Queue Utopia. But in reality, we are seeing an opposite trend: the cost for new drugs per investment dollar is exploding, life expectancy is stagnant or decreasing throughout the developed world, incident rates for many diseases are increasing, and many major illnesses we expected to cure by now seem to have made little to no progress.
You can probably think of many holes to poke in these arguments and potentially other villains. "It’s not a matter of the cost, but the incentives!! There is no money to be made in the cure - only the treatment! This is why Big pharma is of course suppressing the cure for major illnesses like diabetes and cancer."
I’m not a defender of big business, but I can tell you, these treatments are not lurking out there hidden for the average person like you and me. If you don’t believe me, think about the powerful and wealthy people like John McCaine or Steve Jobs that have died from cancer. Surely if there was something out there, they would get it. In a similar vein, do you know how I know there isn’t a cure for hair loss? Because if there was one, Jeff Bezos would have the most impressive head of hair on the planet.
Let’s get back to being serious - the biggest advances in cancer therapeutics have been immunotherapies, and these have been painfully slow to develop and fraught with unexpected challenges and failed clinical studies despite billions of dollars of investment.
Ok, so if big pharma isn’t hiding the cure for cancer, what is going wrong? Moreover, what does this have to do with AI? We will talk about all of this and more throughout the article. But let’s start by identifying the challenges facing Pharma.
Traditional Pharma in a Death Spiral.
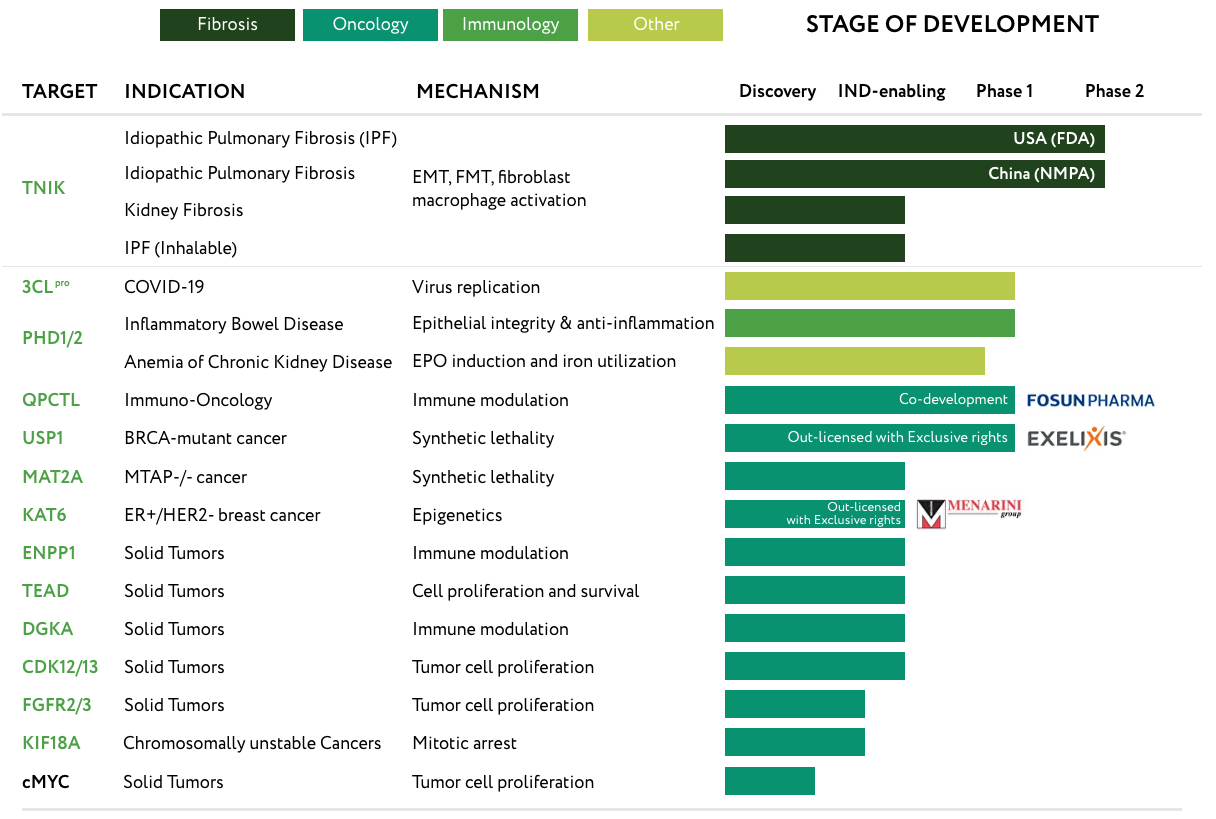
Over the past century, the developmental pipeline for Pharma has become well defined (Figure 1). It begins with discovery and development of new therapeutics, e.g., proteins, antibodies, small molecules etc. These can be discovered either by high-throughput screening or more targeted approaches based on understood mechanisms. These products are then tested in laboratory assays to establish an understanding of the drugs therapeutic window, i.e., the concentration range where it is both efficacious and safe. Promising drugs are then tested in preclincal settings, typically starting with small animals such as laboratory mice and eventually larger mammals such as pigs or canines. Drugs that show enough evidence of safety and therapeutic impact are then submitted to the FDA for regulatory approval of testing in the clinic as an investigational new drug (IND). The clinical study then focuses around testing the product safety and efficacy in stages.
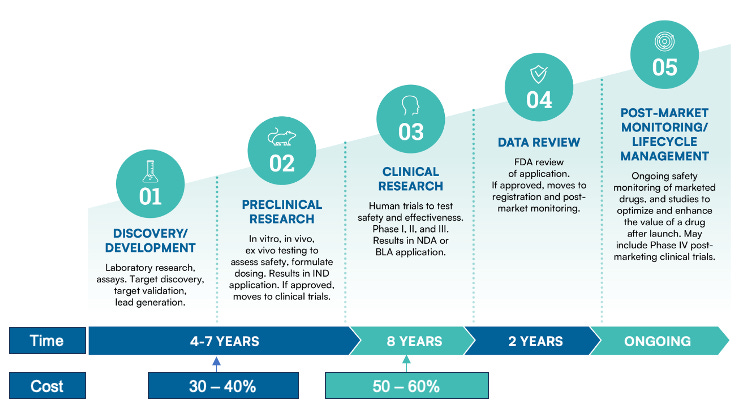
On its face, this production cycle may not seem so complicated and you may wonder where the challenges come from. What better way to highlight these challenges in the biotechnology sector than to juxtapose them with the flourishing technology sector (Table 1).
The development and improvement of computing technology over the past 70+ years has been nothing short of incredible. Moore’s law is the observation of this exponential growth in the number of transistors in an integrated circuit, such that we can be fairly confident it will double every two years. As a result, new computers generally get significantly more powerful and cheaper over time. This is an emergence of modern capitalism where markets optimize products, and the recursive improvements keep this law alive and well.
Table 1. Comparison of Key Challenges in Biotechnology vs. Software Technology (Adapted from ‘Zero to One’).
By contrast, drug discovery has shown a counter trend (Figure 2). Over time, drug development has become slower and much more expensive. In the 1950s, for every $1 billion of investment, we would receive approximately 20-30 new drugs. By 2023, this figure is down to less than one drug per billion dollars of investment. Overall, the probability of a new drug reaching the market is less than 10% with an expectation of 10-15 years to market. This decay in development has been colloquially termed Eroom’s law (Moore’s law spelled backwards).
There are undoubtedly many sources for these challenges. First, the exhaustion of new opportunities (new diseases to treat) with a progressively higher bar for improvement over existing therapies (the low hanging fruit has been picked). At the same time an increasingly conservative regulatory body privileges lives saved by rejecting drugs more than lives lost by slowing down progress. This article could just as easily be written on how government over-regulation and greedy insurance companies have destroyed the pharma industry through cost disease. While there are some elements of truth there, that is not the full story. Biology is hard and messy. In all the ways that software and hardware are neat, controlled systems built by engineers, biology consists of multivariable systems built by nature. So, how can AI reverse this?
Understanding the Basics of Biological Structure and Function in Drug Development:
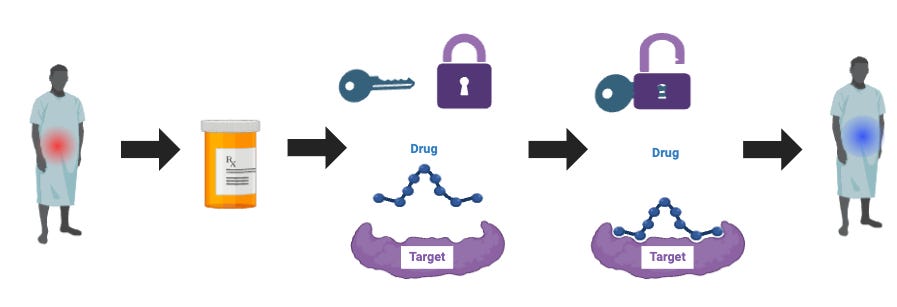
In its simplest form, the central thesis in Pharmaceuticals is that by using a drug in the form of a small molecule, peptide, or protein, we can either send or block a signal in a biological pathway. This will manifest some downstream effect by either activating or inhibiting a physiological response. That’s it. Simple, right? Essentially, these drugs aim to modulate specific pathways in a complex, multifactorial biological system to achieve a desired outcome.
Let’s take the example of coffee and its primary psychoactive ingredient, caffeine. Caffeine is a stimulant, but how does this mechanism work? In the brain, our neurons contain adenosine receptors. As adenosine accumulates through metabolism, it acts on the neurons in our brain, resulting in the feeling of drowsiness. Caffeine blocks the action of adenosine by binding to its receptors, inhibiting its effects of promoting sleep and relaxation.
But why do these molecules bind to specific receptors? A key component in this process is the three-dimensional shape of proteins, enzymes, and other biomolecules. This shape determines how they interact with other molecules. The effectiveness of a drug often hinges on its ability to bind precisely to a biological target, such as a receptor. This interaction can be compared to a ‘lock and key’ mechanism (or more recently re-termed ‘induced-fit’), where the drug (key) must perfectly match the biological target (lock) to elicit the desired effect (Figure 3).
Traditionally, finding these drugs has involved a significant element of luck. Discovery often happens either by accident or by high-throughput screening of thousands of compounds in highly specific assays. This indirect approach is time-consuming, expensive, and lacks specificity. However, advancements in AI are poised to change this paradigm.
Generative AI in Pharma
Generative AI, known for its ability to create content like text and images, is revolutionizing various fields, including pharmaceuticals. This technology leverages deep learning models, particularly neural networks, to understand and replicate complex patterns in existing datasets, producing new, original outputs that maintain fidelity to the learned material.
Why is this important? As discussed earlier, drugs function by inhibiting or activating biological pathways, which depend on their ability to bind to a specific receptor. This requires the drug and site of interest to have complementary shapes to effectively bind. You may be wondering, why can't we just simulate this on a computer? The short answer is, that we’ve been trying, but it turns out to be a very difficult task, at least it had been until the advent of generative AI.
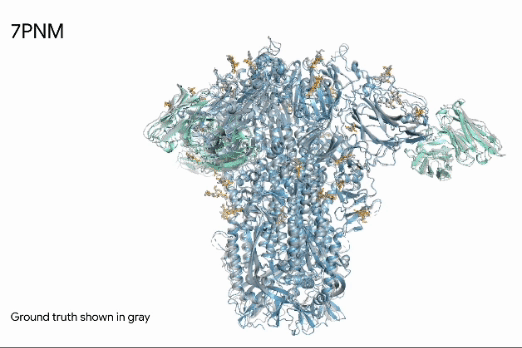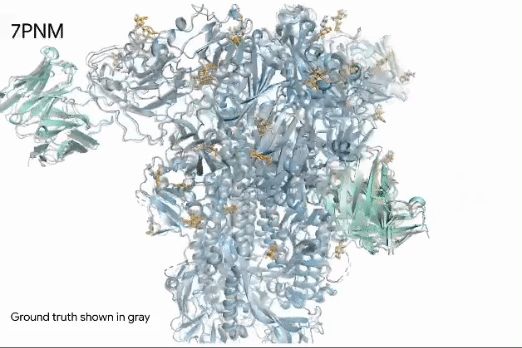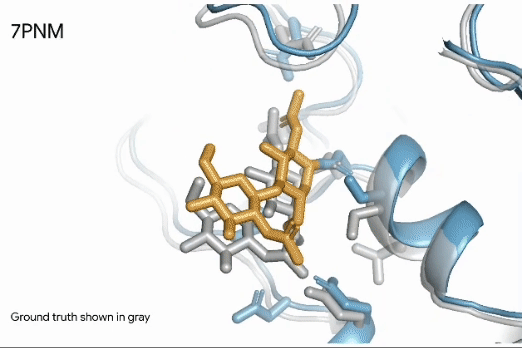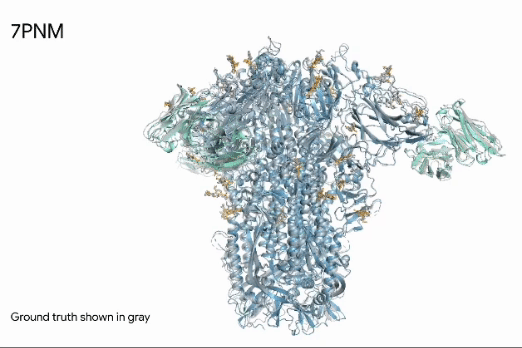
Emerging AI tools are now enabling significant breakthroughs in developing new therapeutics. Generative AI tools allow researchers to model the 3D structure of proteins and other molecules. For example, AlphaFold, developed by DeepMind, predicts the 3D structure resulting from complex amino acid sequences, which fold into intricate, highly-specific shapes (Figure 4). Beyond modeling, these tools can also predict molecules with complementary shapes and a high likelihood of binding, essentially predicting new drugs rather than screening for them (Abramson et al, 2024).
A more comprehensive list of some of these key applications can be found below:
Predictive Modeling of Molecular Structures: Generative AI predicts 3D structures of proteins and biomolecules quickly, aiding drug design by foreseeing interactions and filling experimental data gaps.
Drug Design and Optimization: AI designs new molecules optimized to bind targets effectively, accelerating drug discovery and improving therapeutic specificity and efficacy.
Simulation of Molecular Dynamics: AI simulates molecular interactions over time, offering insights into absorption, metabolism, and excretion, which enhances drug performance and reduces side effects.
Enhancing Selectivity and Reducing Toxicity: AI designs drugs with high selectivity to minimize unintended interactions and side effects, optimizing both the shape and properties of drug molecules.
Personalized Medicine: Generative AI analyzes genetic variations to design personalized drugs, improving treatment efficacy and safety in precision medicine.
As you can see, there is enormous potential in generative AI for predicting new drugs.
Translation of generative AI drug discovery to industry
The use of generative AI seems to have enormous promise. But how is it actually being deployed within the pharma industry?
Let’s take a brief case study: In’silico Medicine
Insilico Medicine is a biotechnology firm based in Hong Kong, and a leader in the field for integrating AI in drug discovery. Their mission is to accelerate the development of new drugs using AI across various stage sof the process including:
Target identification: Insilico’s AI tool, PandaOmics, rapidly identifies and prioritizes drug targets by analyzing extensive biological data. It integrates data from omics studies and clinical datasets to find and validate new targets efficiently.
Molecular simulations: This AI engine designs novel drug candidates by generating chemical structures predicted to bind effectively with identified targets. It uses deep learning models to simulate and optimize molecular interactions, significantly speeding up the drug design process.
Drug properties prediction: The AI predicts the physical and chemical properties of new compounds, aiding in the design of molecules that are more likely to be effective and safe.
Candidate prioritization: AI helps prioritize drug candidates by assessing their predicted efficacy and safety profiles, streamlining the decision-making process for further testing.
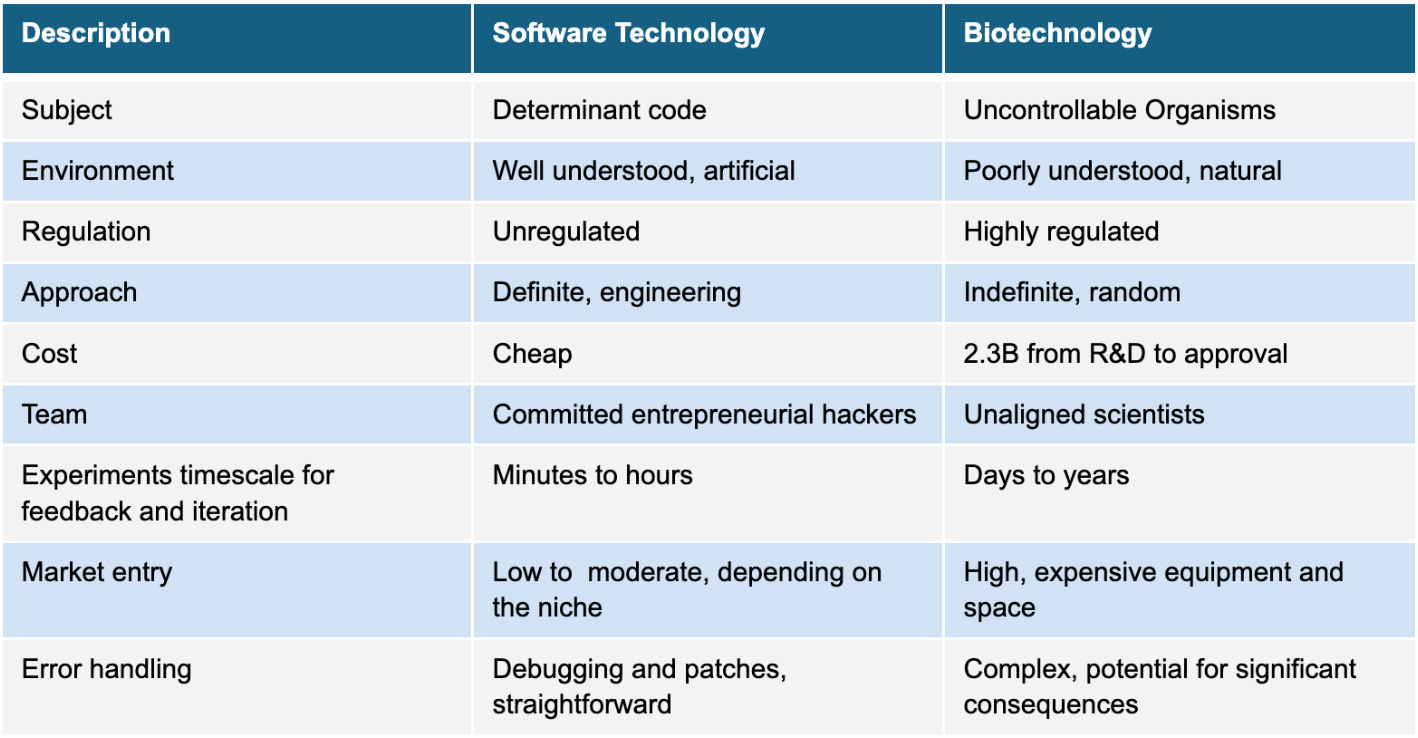
Insilico Medicine’s approach has the potential to streamline the drug synthesis process and target therapeutic development more effectively. They are currently attempting to tackle diseases such as cancer, fibrosis, immune disorders, and central nervous system diseases. For instance, their drug candidate INS018_055 for idiopathic pulmonary fibrosis (IPF) moved from target discovery to Phase I clinical trials in under 30 months. Compare this to the normal 4-7 year timeline discussed in the prior section! This will be an important bellwether in the ability of generative AI to impact pharma to result in faster, cheaper, and more effective therapeutic solutions.
Update: It was recently shared by Insilico Medicine’s CEO, Alex Zhavoronkov, that they received their first Phase IIa readout for their IPF drug INS018_055! The 12-week study enrolled 71 patients across 21 sites in China and assessed both safety and impact on lung function. The trial met its primary endpoints of safety and tolerability at all dose levels. Furthermore, it showed a dose-dependent improvement in a key output: forced vital capacity (FVC), the maximum amount of air a person's lungs can forcefully exhale after their deepest possible inhale. While there is still a way to go to reach the market, these fast and promising results continue to impress.
Beyond Drug Discovery, How can AI Enhance Overall Development?
In silico medicine is undoubtedly already having a major impact in the area of drug discovery. However, it will likely be years before any of these drugs complete their clinical studies. Moreover, drug discovery is only the first step—the clinical studies are the longest and most expensive part of the drug development pipeline. So, is there anything that AI can do about this? The answer is yes. AI can significantly transform clinical studies in several ways, potentially reducing time and costs while increasing efficiency and success rates.
Patient Recruitment and Selection
Recruiting suitable participants is one of the most challenging and time-consuming aspects of clinical trials. Ensuring that the selected participants meet the specific criteria is crucial for the trial's success.
How AI can help:
Enhanced Recruitment: AI algorithms can analyze large datasets, including electronic health records (EHRs), to identify and match eligible patients quickly and accurately.
Predictive Analytics: AI can predict patient eligibility based on their medical history, genetic information, and other relevant data, streamlining the recruitment process.
Example: AI platforms like Deep 6 AI use natural language processing (NLP) to sift through millions of medical records to find eligible patients for clinical trials, reducing recruitment time from months to weeks.
Trial Design and Optimization
Designing a clinical trial involves selecting endpoints, determining sample sizes, and defining protocols—all of which can impact the trial's efficiency and success.
How AI can help:
Simulating Trials: AI can simulate various trial designs to predict outcomes, helping researchers select the most effective and efficient design.
Adaptive Trials: AI can enable adaptive trial designs that allow modifications based on interim results, improving the chances of success.
Example: Cytel's AI-driven platform, Solara, provides simulations to optimize trial designs, helping pharmaceutical companies design more efficient and effective clinical trials.
Monitoring and Managing Trials
Continuous monitoring and management of clinical trials are critical to ensure compliance, data integrity, and patient safety.
How AI can help:
Real-Time Monitoring: AI can monitor ongoing trials in real-time, identifying potential issues early and ensuring adherence to protocols.
Automated Data Collection: AI can automate data collection and analysis, reducing human error and accelerating the process.
Example: AI-powered platforms like Medidata Rave use machine learning to monitor clinical trial data in real-time, identifying anomalies and ensuring data quality.
Predictive Modeling and Outcome Prediction
Predicting the outcomes of clinical trials is complex and uncertain, often leading to failures in later stages.
How AI can help:
Predictive Modeling: AI can build predictive models using historical trial data and patient characteristics to forecast trial outcomes and identify potential risks.
Biomarker Identification: AI can identify biomarkers that predict patient responses to treatments, allowing for better-targeted therapies.
Example: Tempus uses AI to analyze clinical and molecular data, providing predictive insights that help tailor treatments and predict trial outcomes.
Patient Adherence and Engagement
Ensuring that patients adhere to the trial protocols and remain engaged throughout the study is essential for obtaining reliable results.
How AI can help:
Virtual Health Assistants: AI-driven virtual assistants can remind patients to take their medications, track their symptoms, and provide real-time support.
Wearable Devices: AI can analyze data from wearable devices to monitor patient adherence and health status continuously.
Example: Companies like Biofourmis use AI to analyze data from wearables, providing continuous monitoring and personalized feedback to patients, enhancing adherence and engagement.
Conclusion
It's easy to lose track of the things that truly matter. Facing our own mortality or the sickness of someone we care for brings perspective. Randy Pausch, in "The Last Lecture," said, "Time is all you have. And you may find one day that you have less than you think." The capacity to take care of those in need underscores the importance of the pharmaceutical industry. Despite its critical role, the pharmaceutical industry faces significant challenges: the pace of drug development is slowing, while costs and risks continue to rise. Can Moore’s law counteract Eroom’s law?
I believe that the integration of AI into the pharmaceutical industry can revolutionize traditional paradigms of drug discovery and development, making these processes more efficient and precise. AI-driven drug discovery is already showing promise in identifying new drug candidates and optimizing therapeutic designs. Its potential to transform clinical trials is equally significant. AI can streamline patient recruitment, optimize trial designs, enable real-time monitoring, and predict outcomes, thereby reducing the time and costs associated with bringing new drugs to market.
Beyond drug development, AI's applications in precision medicine, medical imaging, and virtual health assistance illustrate its broader impact on healthcare. As AI continues to evolve, it will predictably drive innovations that improve patient outcomes and enhance the efficiency of medical research and delivery. It will take embracing these technological advancements to break Eroom’s law.
Support:
These newsletters take a significant amount of effort to put together and are totally for the benefit of the reader. If you find these explorations valuable, there are multiple ways to show your support:
Engage: Like or comment on posts to join the conversation.
Subscribe: Never miss an update by subscribing to the Substack.
Share: Help spread the word by sharing posts with friends directly or on social media.
References:
Abramson, J., Adler, J., Dunger, J., Evans, R., Green, T., Pritzel, A., Ronneberger, O., Willmore, L., Ballard, A.J., Bambrick, J. and Bodenstein, S.W., 2024. Accurate structure prediction of biomolecular interactions with AlphaFold 3. Nature, pp.1-3.
DiMasi, J. A., Grabowski, H. G., & Hansen, R. W. (2016). Innovation in the pharmaceutical industry: New estimates of R&D costs. Journal of Health Economics, 47, 20-33.
Ren, F., Aliper, A., Chen, J., Zhao, H., Rao, S., Kuppe, C., Ozerov, I.V., Zhang, M., Witte, K., Kruse, C. and Aladinskiy, V., 2024. A small-molecule TNIK inhibitor targets fibrosis in preclinical and clinical models. Nature Biotechnology, pp.1-13.
Ringel, M.S., Scannell, J.W., Baedeker, M. and Schulze, U., 2020. Breaking Eroom’s law. Nat Rev Drug Discov, 19(12), pp.833-834.
Thiel, P. and Masters, B., 2014. Zero to one: Notes on startups, or how to build the future. Crown Currency.
https://www2.deloitte.com/content/dam/Deloitte/ch/Documents/life-sciences-health-care/ch-deloitte-media-release-pharma-innovation-2024-13052024.pdf
https://en.wikipedia.org/wiki/Transistor_count