Happy Monday Morning, Readers. Let’s be relentless this week!
In this week’s edition of BioWire, we’re reviewing a range of interesting and controversial topics at the boundaries of science and technology.
Body Roundness Index as a New Predictor of Mortality
Paternal Diet Influences Metabolic Health of Offspring!
Semaglutide and Risk of Increased Suicidality from WHO Data
GLP-1 Agonists in the Hot Seat with Pricing Battles and Senate Scrutiny
As a quick note, all four topics this week pertain to obesity, whether through the lens of measuring indexes for health outcomes, the heritability of metabolic disorders linked to poor diet, side effects of weight loss drugs, or the regulatory battles surrounding these medications. This thematic overlap wasn’t intentional—I came across each of these topics organically. However, it underscores just how severe the obesity epidemic has become and highlights its rising prominence in scientific research and public health discourse.
Body Roundness Index as a New Predictor of Mortality
Great comedians have this uncanny ability to tell a story, make us laugh, all while revealing a deeper truth. George Carlin, the legendary comedian, had an old bit about how euphemistic language has evolved to soften harsh realities. In his standup, he masterfully traced how the term "shell shock" from World War I evolved through the decades into the sterile "Post-Traumatic Stress Disorder" by the Vietnam War. His point was clear: we often hide behind euphemisms to avoid confronting uncomfortable truths. Nowhere is this more evident than in the global obesity epidemic. Just as we’ve rebranded harsh realities into softer, more palatable terms, we’ve also struggled to accurately measure, address, or even talk about the complex nature of obesity, a major comorbidity that contributes to a wide range of health issues including cardiovascular disease, type 2 diabetes, osteoarthritis, certain cancers, and overall reduced lifespan.
Traditionally, Body Mass Index (BMI) has been the go-to metric for assessing obesity-related health risks. As in the name, this measurement is based on the ratio of weight and height. However, it often falls short in capturing the true complexity of body fat distribution and its impact on health. Visceral fat, the fat stored around internal organs, is particularly harmful, yet BMI doesn’t effectively differentiate between muscle, subcutaneous fat, and visceral fat. As the obesity epidemic continues to weigh on our society, there is a growing need for more accurate measures that can better predict health outcomes associated with body composition.
A recent study published in JAMA Network Open introduces the Body Roundness Index (BRI) as a potentially superior measure of obesity and its association with all-cause mortality, compared to traditional metrics like BMI (Zhang et al., 2024). As the name implies, this index is based on the ratio of waist circumference to height, giving a more comprehensive reflection of body fat distribution, particularly visceral fat. BRI was found to be a stronger predictor of mortality than BMI. One can only imagine Carlin crafting a bit around this shift—from mass to shape—as a fresh lens through which to scrutinize our collective avoidance of uncomfortable truths.
In the study, researchers analyzed data from over 32,000 US adults from the National Health and Nutrition Examination Survey (NHANES) spanning from 1999 to 2018. The findings revealed a U-shaped association between BRI and mortality, indicating that both low and high BRI scores are linked with increased mortality risk. Specifically, individuals with a BRI below 3.4 had a 25% higher risk of death, while those with a BRI of 6.9 or higher faced a 49% increased risk compared to those in the middle BRI range of 4.5 to 5.5. Over the study period, the average BRI increased significantly, with the rise more pronounced among women and the elderly. This trend parallels the broader obesity epidemic, suggesting that BRI might better capture the health risks associated with changes in body composition over time.
These findings show BRI as a promising tool for assessing mortality risk related to body fat distribution, potentially offering a more precise measure for public health and clinical use.
Paternal Diet Influences Metabolic Health of Offspring!
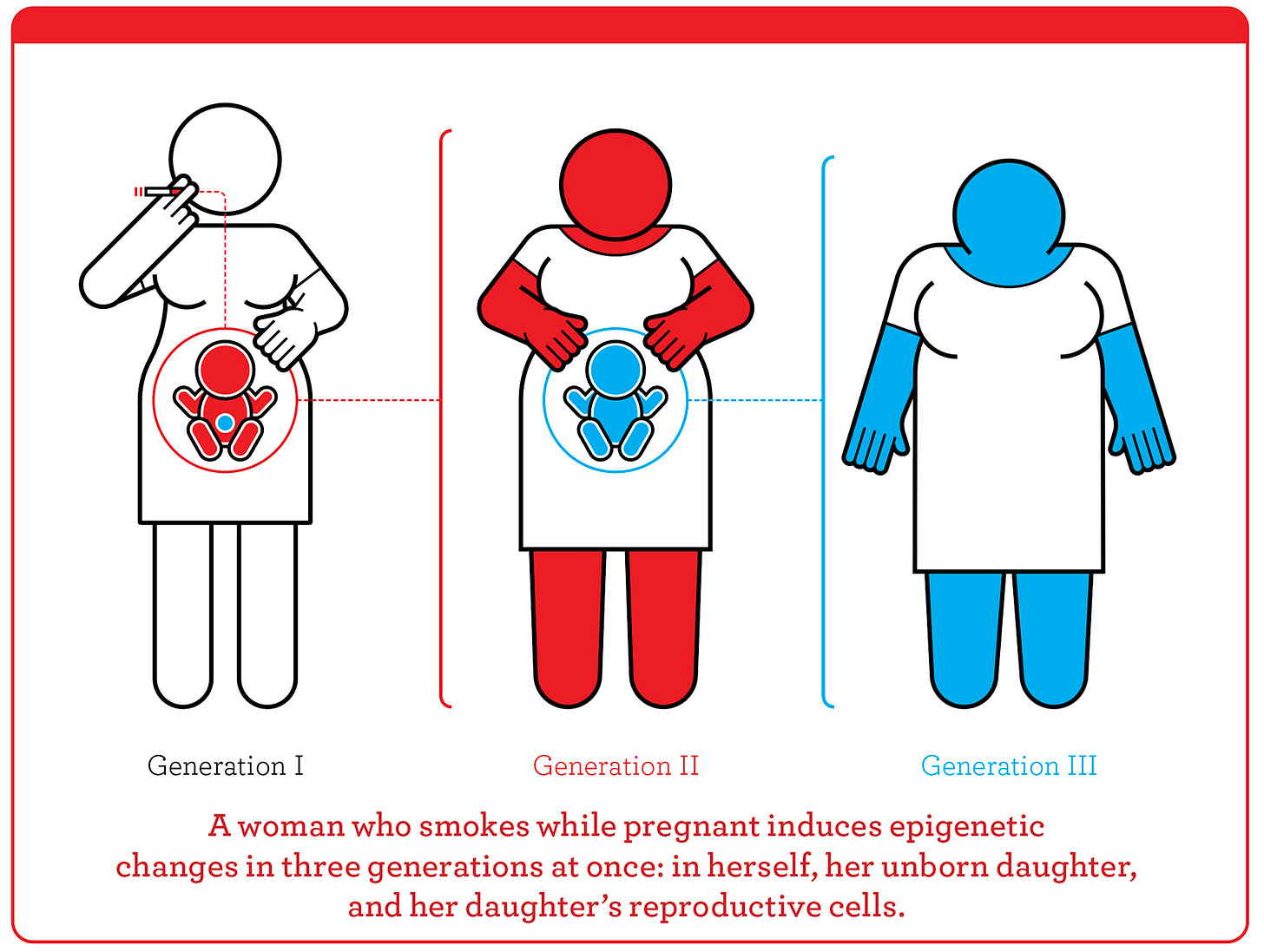
The question of how much our traits are shaped by genetic inheritance versus environmental influences has fascinated scientists for decades. While our genetic code provides the blueprint, it's becoming increasingly clear that our environment can rewrite parts of that script through a process known as epigenetics. This area of study explores how factors like diet, stress, and lifestyle can alter gene expression without changing the underlying DNA sequence itself. For years, the prevailing belief was that these epigenetic changes were not passed on to future generations. But in the early 2000s, a breakthrough challenged this idea: researchers discovered that maternal behavior in rats—specifically the amount of licking and grooming—could cause lasting changes in how their offspring’s genes were expressed, particularly in stress response pathways (Weaver et al., 2004).
As studies continued, the story took another surprising turn. Researchers found that male mice conditioned to fear a specific odor passed this fear on to their offspring (Dias et al., 2014). The pups, and even the next generation, showed heightened sensitivity to the same odor, despite never having been exposed to it themselves. The secret lay in the sperm: epigenetic changes were altering how odorant receptor genes were expressed, showing how a father’s experiences could echo through generations. These findings shattered the notion that epigenetic changes were confined to one lifetime, opening the door to a new understanding of inheritance that goes beyond just DNA.
But how, exactly, do fathers transmit these epigenetic signals? The mechanisms have remained largely mysterious—until now. A recent study published in Nature reveals that a father’s diet can profoundly influence his offspring’s health (Tomar et al., 2024). Researchers fed male mice a high-fat diet (HFD) for just two weeks before conception, and the results were striking. Changes in specific mitochondrial RNAs (mt-tRNAs) were detected in the sperm, acting as messengers that carried environmental information from father to offspring. When these altered RNAs were delivered to the egg at fertilization, they influenced the early development of the embryos. The male offspring of HFD-fed fathers displayed signs of metabolic dysfunction: glucose intolerance and insulin resistance, which are early indicators of metabolic disorders.
What’s especially compelling is the reversible nature of this effect. When the fathers were given time to recover on a normal diet before conception, the metabolic issues in the offspring disappeared, highlighting the immediacy and reversibility of these epigenetic changes. This study underscores the critical impact of paternal health at conception and suggests that sperm mt-tRNAs act as sensors of environmental conditions, transmitting metabolic information to the next generation.
These discoveries push us to rethink the boundaries of inheritance. They show that what fathers eat, how they live, and the environments they are exposed to can leave a biological legacy that shapes their children’s health in ways that were previously unimaginable. This emerging field of research challenges the traditional view of heredity, blending genetics and epigenetics to tell a richer, more complex story of how traits and risks are passed down.
Semaglutide and Risk of Increased Suicidality from WHO Data
Recent findings have raised important questions about the safety profile of popular weight-loss drugs, particularly semaglutide, known by its brand names like Ozempic and Wegovy. While these GLP-1 receptor agonists have gained widespread use for their effectiveness in weight management, a new study analyzing data from the World Health Organization’s global database of suspected adverse drug reactions has detected a concerning signal: semaglutide may be associated with an increased risk of suicidal ideation (Schoretsanitis et al., 2024). This large-scale disproportionality analysis found that reports of suicidal thoughts were significantly higher among patients using semaglutide compared to other medications, especially in those also taking antidepressants or benzodiazepines.
The study did not find a similar signal for liraglutide, another GLP-1 receptor agonist commonly prescribed for weight loss and type 2 diabetes. Researchers identified 107 cases of suicidal and self-injurious behaviors associated with semaglutide, with a notable risk of suicidal ideation, particularly when compared to other drugs like metformin and dapagliflozin. These findings have sparked calls for further investigation, as the use of semaglutide extends beyond diabetes management into off-label and lifestyle contexts, where psychiatric side effects may be underrecognized. The European Medicines Agency (EMA) and the U.S. FDA are already reviewing these drugs for potential psychiatric risks, underscoring the need for heightened awareness among healthcare providers and patients.
As the popularity of GLP-1 agonists continues to rise, balancing their benefits and risks becomes increasingly crucial. Some of these drugs may have distinct advantages in their side effect profiles while offering similar therapeutic benefits, making it essential to evaluate these differences thoroughly as these medications gain broader use. Understanding potential risks, especially for vulnerable populations, is vital to ensuring that these therapies are used safely and effectively.
GLP-1 Agonists in the Hot Seat with Pricing Battles and Senate Scrutiny
In another story about GLP-1 agonists, Eli Lilly's recent price cut for Zepbound and Novo Nordisk's upcoming Senate hearing on Wegovy have put this drug class under intense scrutiny. Lilly's decision to slash Zepbound's price appears to be a strategic move to capture market share from Novo Nordisk's Wegovy, the current market leader in the GLP-1 agonist space. This price cut has sparked discussions on the broader implications for accessibility, competition, and the impact on insurance coverage, potentially setting a new precedent for pricing strategies within the weight-loss drug market.
Meanwhile, Novo Nordisk faces a new challenge: defending Wegovy's pricing in front of the U.S. Senate. As the healthcare costs associated with obesity management continue to rise, the Senate hearing aims to address the affordability and accessibility of these medications. The scrutiny comes amidst increasing pressure on pharmaceutical companies to justify the high prices of blockbuster drugs, particularly those that target widespread conditions like obesity and diabetes. Novo Nordisk's testimony could influence not just Wegovy’s pricing but also the regulatory landscape for weight-loss treatments, making it a pivotal moment for the industry.
These developments underscore the growing tension between innovation and affordability in the biopharmaceutical landscape. As major players like Lilly and Novo Nordisk navigate the complexities of market competition and regulatory oversight, the outcomes of these actions could shape the future of weight-loss therapeutics, making the stakes higher than ever for both companies and patients.
Support:
These newsletters take a significant amount of effort to put together and are totally for the benefit of the reader. If you find these explorations valuable, there are multiple ways to show your support:
Engage: Like or comment on posts to join the conversation.
Subscribe: Never miss an update by subscribing to the Substack.
Share: Help spread the word by sharing posts with friends directly or on social media.
References:
https://www.biospace.com/business/with-lillys-zepbound-price-cut-and-novos-impending-senate-hearing-wegovy-is-in-the-hot-seat
https://www.harvardmagazine.com/2017/04/is-epigenetics-inherited
Dias, B.G. and Ressler, K.J., 2014. Parental olfactory experience influences behavior and neural structure in subsequent generations. Nature neuroscience, 17(1), pp.89-96.
Schoretsanitis, G., Weiler, S., Barbui, C., Raschi, E. and Gastaldon, C., 2024. Disproportionality analysis from World Health Organization data on semaglutide, liraglutide, and suicidality. JAMA Network Open, 7(8), pp.e2423385-e2423385.
Tomar, A., Gomez-Velazquez, M., Gerlini, R., Comas-Armangué, G., Makharadze, L., Kolbe, T., Boersma, A., Dahlhoff, M., Burgstaller, J.P., Lassi, M. and Darr, J., 2024. Epigenetic inheritance of diet-induced and sperm-borne mitochondrial RNAs. Nature, pp.1-8.
Weaver, I.C., Cervoni, N., Champagne, F.A., D'Alessio, A.C., Sharma, S., Seckl, J.R., Dymov, S., Szyf, M. and Meaney, M.J., 2004. Epigenetic programming by maternal behavior. Nature neuroscience, 7(8), pp.847-854.
Zhang, X., Ma, N., Lin, Q., Chen, K., Zheng, F., Wu, J., Dong, X. and Niu, W., 2024. Body Roundness Index and All-Cause Mortality Among US Adults. JAMA Network Open, 7(6), pp.e2415051-e2415051.





On the issue of obesity, from a psychological perspective, it is often a symptom of poor emotional regulation. A lot of the time Binge Eating Disorder goes unchecked because people, especially family and friends, tiptoe around the topic as a personal choice. The individual's behavioural patterns, like avoidance, may drive their environment to adopt body shape acceptance practices.
For the lay onlookers, it's easy to blame the obese for their condition; they don't eat right or don't exercise enough. But we know socio-economic status plays a role, just like parental education, air pollution, and so many factors that funnel into macro and micro environmental, behavioural, and genetic phenotypes.
Obesity should be treated as a public health issue just like smoking, drugs, alcoholism. If we keep avoiding talking about it, we may miss signs of emotional struggle that often lead to worse outcomes (e.g. suicide).
An interesting point about extreme obesity is that several contestants on My 600lb Life, many of whom were well over 600 pounds, managed to lose 30-80% of their body weight (200-500lbs), yet still passed away shortly after their significant weight loss. This demonstrates how devastating obesity can be on the body, even after a substantial reduction in weight. Taking preventative measures early is always the best approach, eat healthy, and exercise! A majority of them died at the exact age of 49 or 51, the body probably can't handle much extreme conditioning around that age.